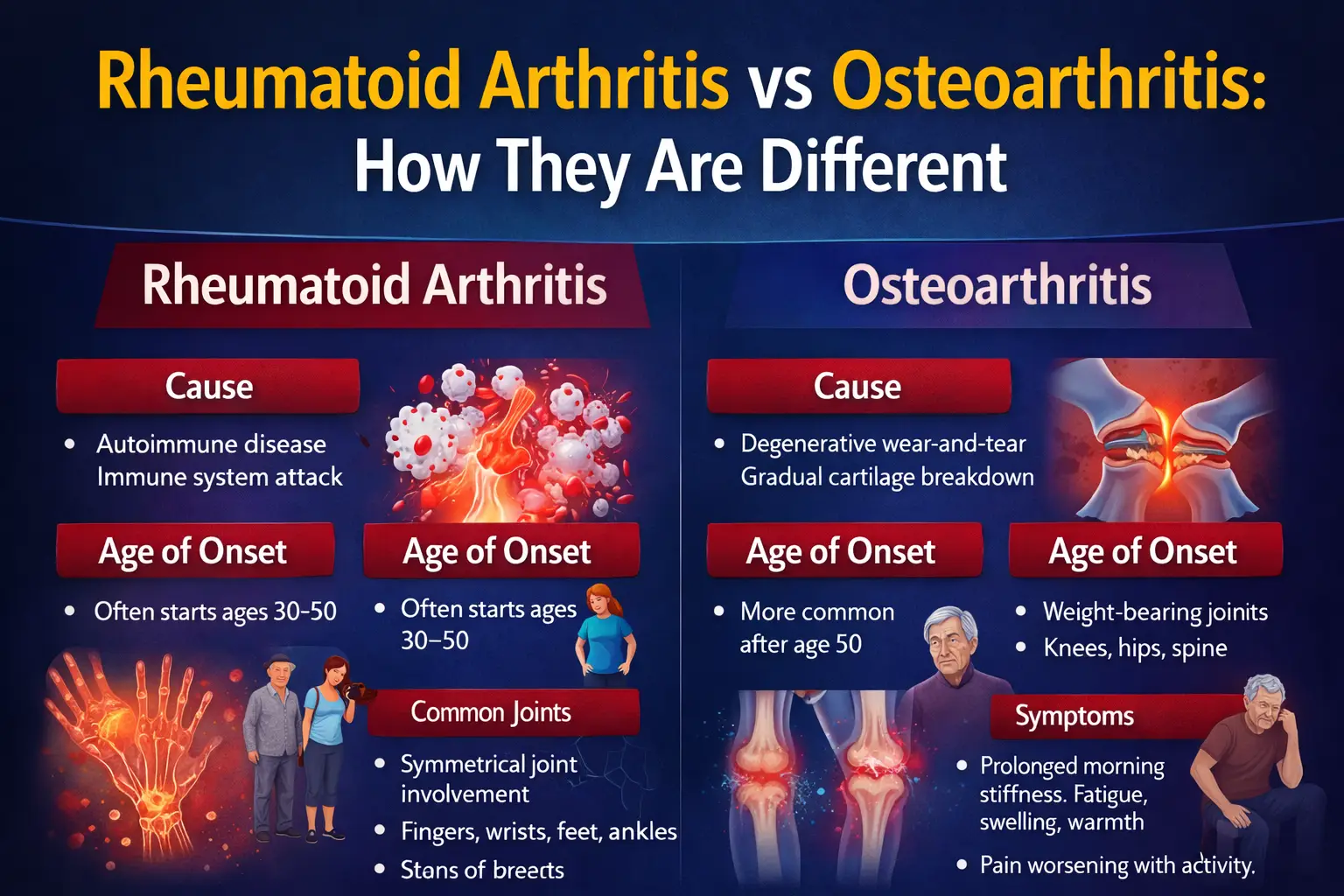
Rheumatoid Arthritis vs Osteoarthritis
Understanding the crucial differences between these two joint conditions — their causes, symptoms, diagnosis, and treatment approaches — to guide your path to recovery
Joint pain is one of the most common reasons people visit a clinic. However, not all arthritis is the same. Two of the most frequently diagnosed joint conditions are rheumatoid arthritis (RA) and osteoarthritis (OA). Although both cause pain, stiffness, and difficulty moving joints, they have very different causes, symptoms, and treatment approaches.
Understanding the difference between RA and OA helps patients seek the right treatment at the right time. Many patients initially assume all joint pain is due to aging — a potentially harmful delay in diagnosis for those with rheumatoid arthritis.
Quick Navigation
A Common Clinical Scenario
Two Patients, Two Very Different Conditions
Presenting complaint: Pain in both hands, with fingers feeling extremely stiff in the morning. Takes nearly an hour before she can comfortably hold a cup of tea. Swelling noticed around knuckles.
Likely diagnosis: Rheumatoid arthritis — an autoimmune inflammatory joint disease requiring early treatment.
Presenting complaint: Knee pain while climbing stairs. Knees hurt after walking long periods but improve with rest. No morning stiffness.
Likely diagnosis: Osteoarthritis — a degenerative wear-and-tear condition developing gradually with age.
Both patients have joint pain, but their underlying conditions, treatment needs, and long-term outcomes are very different.
"How do I know if my joint pain is due to aging or something more serious?" This is one of the most important questions we address at StepUp Joints, Lajpat Nagar. The answer requires proper evaluation.
What is Rheumatoid Arthritis?
Rheumatoid arthritis is a chronic autoimmune disease in which the immune system mistakenly attacks the joints.
How RA Damages Joints
In RA, the immune system targets the synovium, the protective lining of the joints. This triggers:
- Persistent joint inflammation — the root cause of damage
- Swelling and tenderness in affected joints
- Pain and stiffness that worsen with inactivity
- Gradual damage to cartilage and bone if left untreated
Key Difference from OA
Unlike osteoarthritis, rheumatoid arthritis is NOT caused by aging or wear and tear. It is an autoimmune condition where the body's immune system malfunctions and attacks healthy joint tissue.
Who Can Develop RA?
RA can affect:
- Young adults and middle-aged individuals
- Occasionally teenagers
- Women approximately 2–3 times more commonly than men
Without proper treatment, chronic inflammation can progress to joint deformity and disability. However, with early diagnosis and modern medications, most patients achieve excellent disease control and maintain normal, active lives.
What is Osteoarthritis?
Osteoarthritis is the most common type of arthritis worldwide. It is a degenerative joint disease that develops when protective cartilage covering bone ends gradually wears away.
How OA Develops
Cartilage normally acts as a shock absorber in the joint, protecting bones from friction. When cartilage breaks down, bones begin rubbing against each other directly, causing pain, stiffness, and dysfunction.
Commonly Affected Joints
- Knees
- Hips
- Spine
- Hands and fingers
- Big toe
Risk Factors for OA Development
Osteoarthritis typically develops in:
- People over age 50 — age is the primary risk factor
- Individuals with previous joint injuries — trauma accelerates cartilage breakdown
- People with obesity — excess weight strains joints
- Those with repetitive joint stress — occupational or sports-related
Key Difference from RA
Unlike rheumatoid arthritis, osteoarthritis is NOT an autoimmune condition. It is purely mechanical — a result of cumulative wear and tear on joints over years.
Rheumatoid Arthritis vs Osteoarthritis: Key Differences
Although both conditions cause joint pain, several important differences help doctors distinguish between them and determine the correct treatment.
| Factor | Rheumatoid Arthritis (RA) | Osteoarthritis (OA) |
|---|---|---|
| Primary Cause | Autoimmune disease (immune system attacks joints) | Degenerative wear-and-tear condition |
| Underlying Process | Chronic inflammation of joint lining | Gradual cartilage breakdown |
| Typical Age of Onset | 30–50 years (can occur earlier) | 50+ years (increases with age) |
| Joint Pattern | Symmetrical (both sides of body affected equally) | Asymmetrical (one joint often worse than the other) |
| Morning Stiffness Duration | Prolonged (30–60+ minutes) | Brief (usually under 20 minutes) |
| Joint Swelling Type | Soft, warm, tender swelling (significant inflammation) | Hard, bony enlargement (mild inflammation) |
| Whole-Body Symptoms | Yes — fatigue, fever, weight loss, body aches | No — joint pain only |
| Disease Progression | Can cause rapid joint damage if untreated | Develops slowly over years |
Breaking Down Each Difference
Seek medical evaluation immediately if you experience:
- Persistent joint swelling lasting more than 2 weeks
- Morning stiffness lasting more than 30 minutes
- Pain in multiple joints simultaneously
- Difficulty making a fist or performing normal hand movements
- Joint warmth, redness, or tenderness
- Unexplained fatigue accompanying joint pain
These symptoms may indicate inflammatory arthritis (RA) and require evaluation by a rheumatologist. Many patients unfortunately delay seeking care, assuming pain is due to age or calcium deficiency — a mistake that can allow joint damage to progress.
How Arthritis is Diagnosed
Accurate diagnosis requires a combination of clinical evaluation, laboratory testing, and imaging studies. At StepUp Joints Lajpat Nagar, we use a systematic approach to distinguish between RA and OA and rule out other conditions.
1. Clinical Examination
During consultation, doctors assess:
- Pattern of joint involvement (symmetrical vs. asymmetrical)
- Presence and quality of swelling (soft vs. bony)
- Joint tenderness and warmth
- Range of motion in affected joints
- Duration and severity of morning stiffness
- Associated systemic symptoms
A detailed clinical examination often provides the most important diagnostic clues. This is why seeing an experienced rheumatologist matters.
2. Blood Tests (For Suspected RA)
Several blood markers help confirm autoimmune arthritis:
- Rheumatoid Factor (RF) — positive in 70–80% of RA patients
- Anti-CCP Antibodies — more specific for RA; present early in disease
- ESR and CRP — markers of inflammation levels
- ANA — screens for other autoimmune conditions
Note: OA does NOT show these inflammatory markers, making blood tests a key differentiator.
3. Imaging Studies
Imaging evaluates joint damage and confirms diagnosis:
- X-rays — show bone changes, cartilage loss (OA) or erosive damage (RA)
- Ultrasound of joints — detects fluid, synovial swelling, early damage
- MRI — in selected cases for detailed soft tissue assessment
At StepUp Joints, these investigations can usually be coordinated quickly, allowing patients to receive a clear diagnosis without unnecessary delays.
Early diagnosis is critical, especially for RA. If clinical suspicion is high, start investigating immediately. Delaying blood tests or imaging in hope that symptoms resolve on their own can result in irreversible joint damage.
Treatment Approaches Are Very Different
Because RA and OA have different underlying causes, their treatment strategies are fundamentally different. One-size-fits-all pain management is inadequate for RA.
Rheumatoid Arthritis Treatment
The goal of RA treatment is to control the immune system and prevent joint damage. Early aggressive treatment significantly improves outcomes.
Modern treatments include:
- Disease-Modifying Anti-Rheumatic Drugs (DMARDs) — slow disease progression and prevent joint damage (e.g., methotrexate)
- Biologic medications — target specific immune pathways (TNF inhibitors, IL-6 inhibitors)
- Targeted anti-inflammatory therapies — newer agents with fewer side effects
- Supportive care — physiotherapy, rest during flares, pain management
With early diagnosis and modern treatment, many RA patients achieve remission or low disease activity and live normal, active lives without progressive joint damage.
Osteoarthritis Treatment
OA treatment focuses on reducing pain, improving function, and slowing degeneration. Since OA is degenerative, the goal is symptom management and activity optimization.
Management approaches include:
- Physiotherapy and strengthening exercises — maintain muscle support around joints
- Weight management — reduce mechanical stress on joints
- Pain relief medications — NSAIDs, paracetamol, topical agents
- Joint injections — corticosteroids or hyaluronic acid in selected patients
- Activity modification — avoid high-impact activities, use assistive devices if needed
- Joint replacement surgery — in advanced cases affecting quality of life
OA treatment is individualized and focused on maintaining function and quality of life, not preventing disease progression (which is inherent to the condition).
Importance of Multidisciplinary Care
Joint diseases, especially RA, often require expertise from multiple specialists working together for optimal outcomes.
At StepUp Joints Lajpat Nagar, patients may benefit from collaboration between:
- Rheumatologists — diagnose and manage inflammatory arthritis
- Physiotherapists — restore function through targeted rehabilitation
- Orthopaedic surgeons — surgical intervention if needed
- Pain management specialists — optimize pain control strategies
- Nutrition experts — guide anti-inflammatory diet choices
- Rehabilitation professionals — long-term recovery support
This multidisciplinary approach ensures: Comprehensive disease understanding, optimal treatment strategy, better pain control, faster functional recovery, and improved long-term quality of life.
Why Early Diagnosis Matters
One of the most important messages patients should understand:
Not all arthritis is the same. While osteoarthritis develops slowly over many years, rheumatoid arthritis can cause irreversible joint damage much earlier if untreated. Delaying RA diagnosis by even a few months can result in permanent joint changes.
The Difference Early Treatment Makes
Fortunately, modern medicine has significantly improved RA outcomes. With early diagnosis by an inflammatory arthritis specialist, most patients with RA can:
- Control inflammation — achieve remission or low disease activity
- Prevent joint deformity — avoid permanent damage through early DMARDs
- Maintain normal mobility — continue sports, activities, work
- Avoid disability — preserve independence and quality of life
The Cost of Delay
Delayed diagnosis increases:
- Risk of permanent joint erosion
- Risk of deformity requiring surgery
- Duration of suffering and functional loss
- Need for more aggressive later treatment
Early attention to joint symptoms can make a significant difference — not just in reducing pain, but in preserving mobility and quality of life for years to come.
Frequently Asked Questions
RA is an autoimmune disease where the immune system attacks joint linings, causing chronic inflammation. OA is a degenerative condition caused by gradual wear and tear of protective cartilage. RA can affect anyone at any age and requires early medical treatment. OA typically develops after age 50 due to aging and mechanical stress.
Early RA symptoms include:
- Prolonged morning stiffness (30–60+ minutes) that affects function
- Soft, warm swelling in joints (especially fingers, wrists, feet)
- Symmetrical joint pain (both sides of body affected)
- Fatigue disproportionate to activity level
- Low-grade fever or malaise
- Difficulty with fine motor tasks like making a fist
If you notice these symptoms lasting more than 2 weeks, seek evaluation immediately.
Blood tests are important but not diagnostic on their own. Tests like Rheumatoid Factor and Anti-CCP antibodies support the diagnosis but must be interpreted alongside clinical findings and imaging. Some patients have positive blood tests without symptoms, while others have RA with negative initial antibodies (seronegative RA). A rheumatologist combines clinical examination, blood tests, and imaging for accurate diagnosis.
OA most commonly affects weight-bearing and frequently-used joints:
- Knees — most common, especially with obesity or previous injury
- Hips — significant impact on walking and mobility
- Spine — cervical and lumbar regions
- Hands — especially thumb base and finger joints
- Big toe — first metatarsophalangeal joint
OA typically affects one or a few joints asymmetrically, unlike RA which is symmetrical.
Modern RA treatment uses disease-modifying approaches:
- DMARDs (Disease-Modifying Anti-Rheumatic Drugs) like methotrexate that slow disease and prevent joint damage
- Biologic medications targeting specific immune pathways (TNF inhibitors, IL-6 inhibitors)
- Targeted synthetic agents — newer therapies with better tolerability
- Supportive care — physiotherapy, rest during flares, pain relief
Early, aggressive treatment significantly improves outcomes. Most modern RA patients achieve remission or low disease activity with minimal disability.
Seek rheumatologist evaluation if you experience:
- Morning stiffness lasting more than 30 minutes
- Swelling in multiple joints
- Joint pain persisting for several weeks despite rest
- Joint warmth, redness, or tenderness
- Difficulty with daily activities (making a fist, opening jars, climbing stairs)
- Unexplained fatigue accompanying joint symptoms
Don't wait and assume it's "just aging." Early evaluation is crucial, especially if you suspect inflammatory arthritis. Delays in RA diagnosis can result in permanent joint damage within months.
Yes, though uncommon. Some patients develop OA in certain joints due to wear and tear, while simultaneously having RA in other joints. This requires careful clinical and radiological assessment to distinguish the two conditions and tailor treatment accordingly. If you suspect this, specialist evaluation is essential.
Take-Home Message
Joint pain is common, but the underlying cause matters enormously.
Osteoarthritis is a wear-and-tear condition that develops gradually with age and joint stress. Rheumatoid arthritis is an autoimmune disease that causes persistent inflammation and requires early medical treatment.
If you notice prolonged morning stiffness, swelling in multiple joints, or persistent joint pain lasting several weeks — consult a rheumatologist for proper evaluation and treatment.
Early attention to joint symptoms can make a significant difference — not just in reducing pain, but in preserving mobility and quality of life for years to come.